Your Pelvic Floor Doesn't Live in Isolation: Why treating pelvic health means looking at everything from your breath to your big toe.
Pelvic Floor Physical Therapy in Holly Springs, NC
Your Pelvic Floor Doesn't Live in Isolation:
Why treating pelvic health means looking at everything from your breath to your big toe.
If you've ever Googled "pelvic floor exercises," you've probably landed on a page telling you to do Kegels. Squeeze and hold. Repeat ten times. Done. And while Kegel exercises have their place, this advice misses something enormous: your pelvic floor is not an island. It is not a single muscle group you can fix by contracting it in isolation a few times a day. It is part of a deeply interconnected system — one that includes your breath, your hips, your spine, your nervous system, and even the way you carry stress in your jaw.
This is the foundation of whole-body pelvic floor care, and it's the approach that actually gets people better.
What the pelvic floor actually is
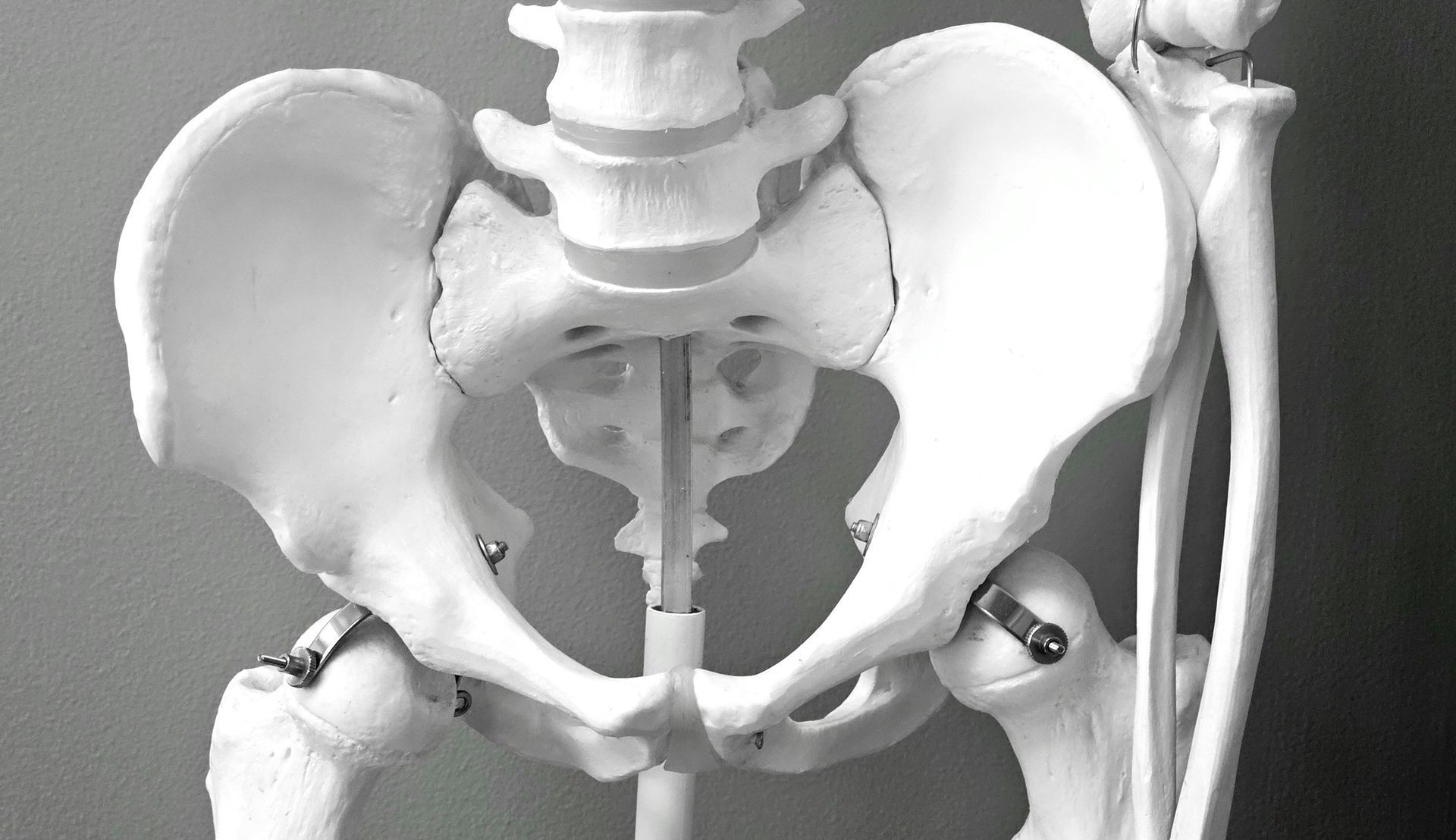
Let's start with the basics, because this is where most people are working from incomplete information. The pelvic floor is a group of muscles and connective tissue that forms a hammock-like structure at the base of your pelvis. These muscles support your bladder, bowel, and uterus (if you have one). They help control urination and bowel movements, contribute to sexual function, and play a major role in stabilizing your pelvis and lower spine during everyday movement.
But here's what most people don't hear: the pelvic floor is in constant conversation with the rest of your body. It contracts and releases in coordination with your diaphragm — the primary breathing muscle — your deep abdominals, and your deep spinal stabilizers. Together, these form what researchers call the "inner unit" of your core. When one part of this system is off, the others feel it.
The pelvic floor responds to your breath, your posture, your movement patterns, and your nervous system state. Treating it in isolation is a bit like tuning one string and calling the guitar fixed.
The breath connection nobody talks about
Breathing is the most overlooked piece of pelvic floor rehabilitation, and it is also one of the most powerful. When you inhale, your diaphragm descends, your ribcage expands, and your pelvic floor naturally lengthens and lowers in response. When you exhale, the diaphragm rises, and the pelvic floor gently lifts. This coordinated rhythm happens thousands of times a day — or it's supposed to.
Many people are chronic breath-holders, chest breathers, or belly tensers. Some have learned to hold their core rigid all day in the pursuit of a "flat stomach." These habits disrupt the natural pressure dynamics in the abdomen and pelvis. Over time, this can contribute to pelvic floor dysfunction — whether that shows up as leakage, prolapse, pelvic pain, or difficulty with bowel movements. Teaching someone to breathe well, fully, and without bracing is often one of the first and most impactful interventions in pelvic floor therapy.
Hips, spine, and the whole kinetic chain
The pelvic floor sits at the intersection of the spine and the hips. It makes sense, then, that tension or weakness anywhere along this chain can affect pelvic floor function. Hip tightness — particularly in the obturator internus, a muscle that lives right at the edge of the pelvic bowl — can pull on the pelvic floor and create a resting tension that makes it impossible to fully relax. A stiff thoracic spine can alter the way load is transferred through the trunk, increasing pressure on pelvic structures below. Even the feet matter: how you strike the ground changes how force travels up through the ankles, knees, hips, and into the pelvis.
This is why a thorough pelvic floor evaluation looks at far more than the pelvic floor itself. A good pelvic PT will assess how you stand, how you walk, how your hip flexors and glutes are functioning, and whether there are movement compensations that are creating downstream (or upstream) problems for your pelvic floor.
The nervous system
Perhaps the most underappreciated factor in pelvic floor health is the nervous system. The pelvic floor has an exceptionally rich nerve supply, and it is exquisitely sensitive to threat and stress. When your nervous system is in a heightened state — anxious, overwhelmed, or braced for impact — your pelvic floor often reflects that. Chronic pelvic pain, for example, frequently involves a nervous system that has learned to interpret normal sensations as dangerous. The muscles guard, the tissues become sensitized, and the cycle of pain and tension perpetuates itself.
A note on hypertonic vs. hypotonic pelvic floors: Not everyone with pelvic floor dysfunction needs to strengthen. Many people — particularly those with pelvic pain, painful intercourse, or certain types of constipation — have pelvic floors that are too tight, not too weak. Kegels for a hypertonic pelvic floor is like stretching an already overstretched rubber band. Part of the whole-body approach is accurately identifying what the pelvic floor actually needs, which requires a proper assessment.
Addressing the nervous system component might involve breathwork, gentle movement, education about pain science, or even working with a therapist who specializes in the mind-body connection. It means helping the nervous system learn that safety is possible — and watching the pelvic floor follow.
What whole-body treatment actually looks like
In practice, a whole-body approach to pelvic floor care means your physical therapist is asking questions that might surprise you. How do you sleep? What does your stress load look like? Do you feel the urge to urinate even when you've just gone, and does that urgency feel more like anxiety than physical pressure? Do you hold your breath when you lift something heavy? Do you feel tension in your jaw or shoulders?
It means treatment might include hands-on work to release hip or thoracic restrictions before ever addressing the pelvic floor directly. It might include breathing exercises before strengthening exercises. It might include education about how to manage intra-abdominal pressure during daily tasks like lifting, sneezing, and exercise — because the way you breathe and brace during these moments matters enormously for pelvic floor load.
And it means that when the pelvic floor work itself does happen, it is thoughtful. It is calibrated to what your body actually needs, not a generic protocol. Strengthening if there is weakness or poor motor control. Downtraining and relaxation if there is excess tension. Coordination work if the timing of muscle activation is off. Often, all three in different proportions.
Why this matters for you
Whether you're dealing with urinary leakage, pelvic pain, recovery after childbirth, prolapse symptoms, painful sex, or simply a vague sense that something is off — you deserve care that sees the whole picture. The pelvic floor is part of you, not separate from you. It responds to how you move, how you breathe, how you manage stress, and how you live in your body day to day.
The good news is that when you approach pelvic floor care from the whole body, the results tend to be more durable. You're not just managing a symptom. You're addressing the conditions that allowed the problem to develop — and building a body that functions better across the board.
So if you've been doing Kegels for months and not seeing results, it might not be that you're doing them wrong. It might be that Kegels aren't the whole answer. Come talk to us. There's a lot more we can do.