Abdominophrenic Dyssynergia: What is it and How Physical Therapy Can Help
Physical Therapy for Abdominophrenic Dyssnergia in Holly Springs, NC

A patient presented to our clinic with a chronic history (greater than 15 years) of GI discomfort, bloating and pain. He was seen by multiple different physicians and prescribed GI medications to help with heartburn and acid reflux. Nothing seemed to change his symptoms. He received numerous tests and scans with no specific outcomes or diagnosis. Unfortunately, he continued to suffer, having to eat smaller portions at a significantly slowed speed and his relationship with food was surrounded by pain and discomfort.
Frustrated with the medical system and desperate for help, he completed his own research which led him to explore more about abdominophrenic dyssynergia.
Abdominophrenic dyssynergia (APD) is a faulty breathing and abdominal muscle pattern where the diaphragm and abdominal wall don’t coordinate the way they should.
Normally: as we inhale the diaphragm contracts to descend downward, abdominals and pelvic floor relax. As we exhale: diaphragm relaxes upward and abdominal wall gently engages.
With APD: we see a paradoxical pattern. As we exhale the diaphragm contracts downward and the abdominal wall stays relaxed. Causing bloating to often be more muscular and pressure related, not digestive.
APD can happen for many different reasons:IBS, pelvic floor dysfunction, postpartum core changes, history of abdominal surgery, chronic stress or shallow breathing, and/or persistent “belly gripping” or abdominal bracing habits.
What have we worked on in Physical Therapy:
- Breathing Retraining: 360 breathing, rib cage expansion and controlled exhale with gentle abdominal engagement
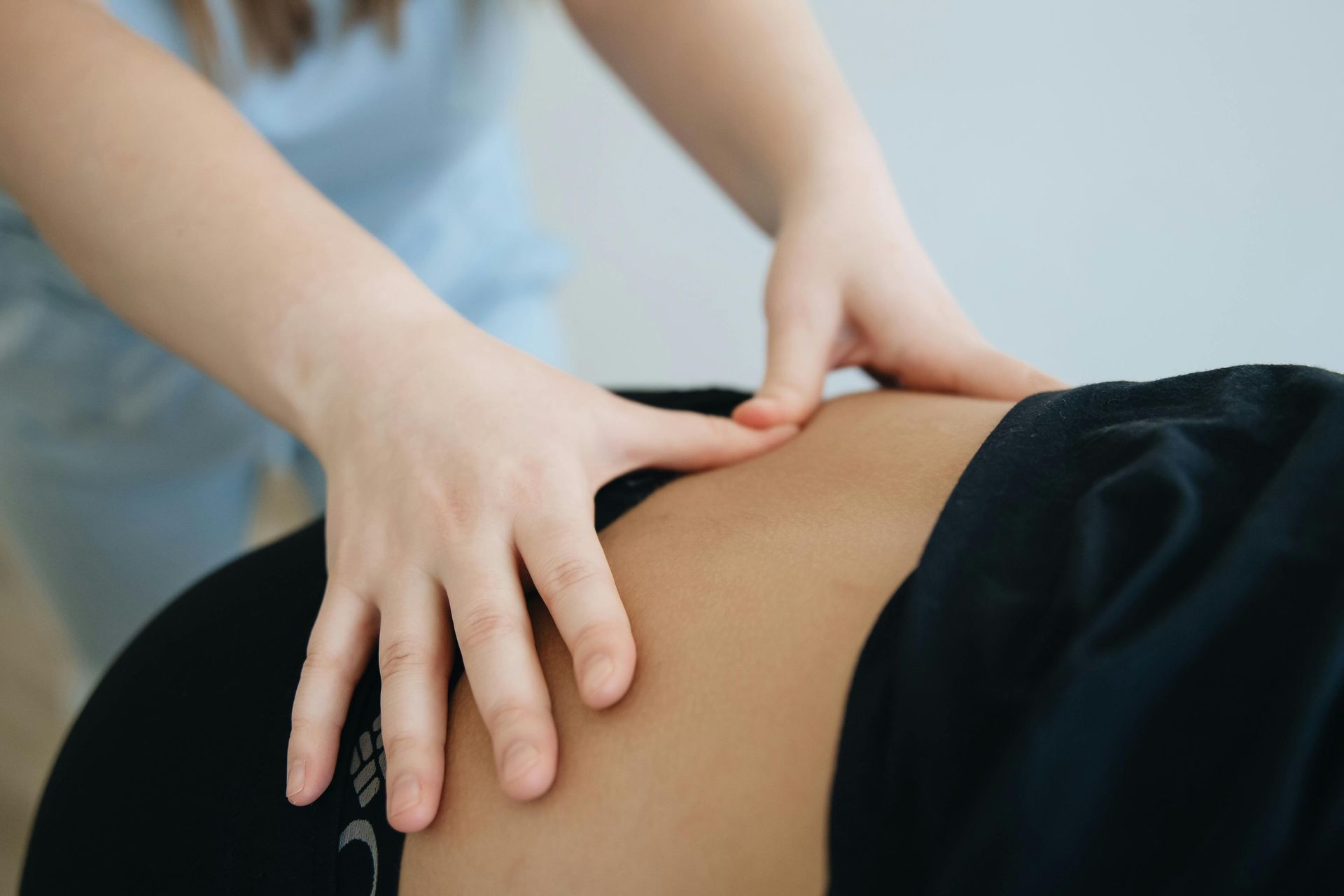
- Abdominal Wall Coordination: deep core activation (transverse abdominis), timing with breathing and relaxation when appropriate
- Posture and Rib Mobility: improving thoracic and rib mobility through manual therapy and postural retraining
- Nervous System Regulation: slow breathing drills, parasympathetic activation and education to improve the gut-brain connection
This patient has been attending physical therapy once a week 6 weeks and is now being treated bi-weekly. He reports decreased bloating, improved speed of eating and decreased pain during and after eating. He states that his relationship with food and overall meal experiences have improved. He now has confidence that his symptoms can improve and be controlled.
If you have been dealing with constant unexplained bloating and nothing has helped it’s not just how your body is and you do not just have to deal with it. APD is common and treatable just often overlooked. Physical therapy may be the answer.
Nicole Perna PT, DPT
Evolve Physical Therapy